Marketing Analytics Built for healthcare
From a compliance headache to confident HIPAA-safe marketing in no time
Custom BAA, HIPAA-certified infrastructure, and guided onboarding – your path to compliance and higher marketing ROI starts here.
US hosting
SOC 2 Type II
ISO 27001
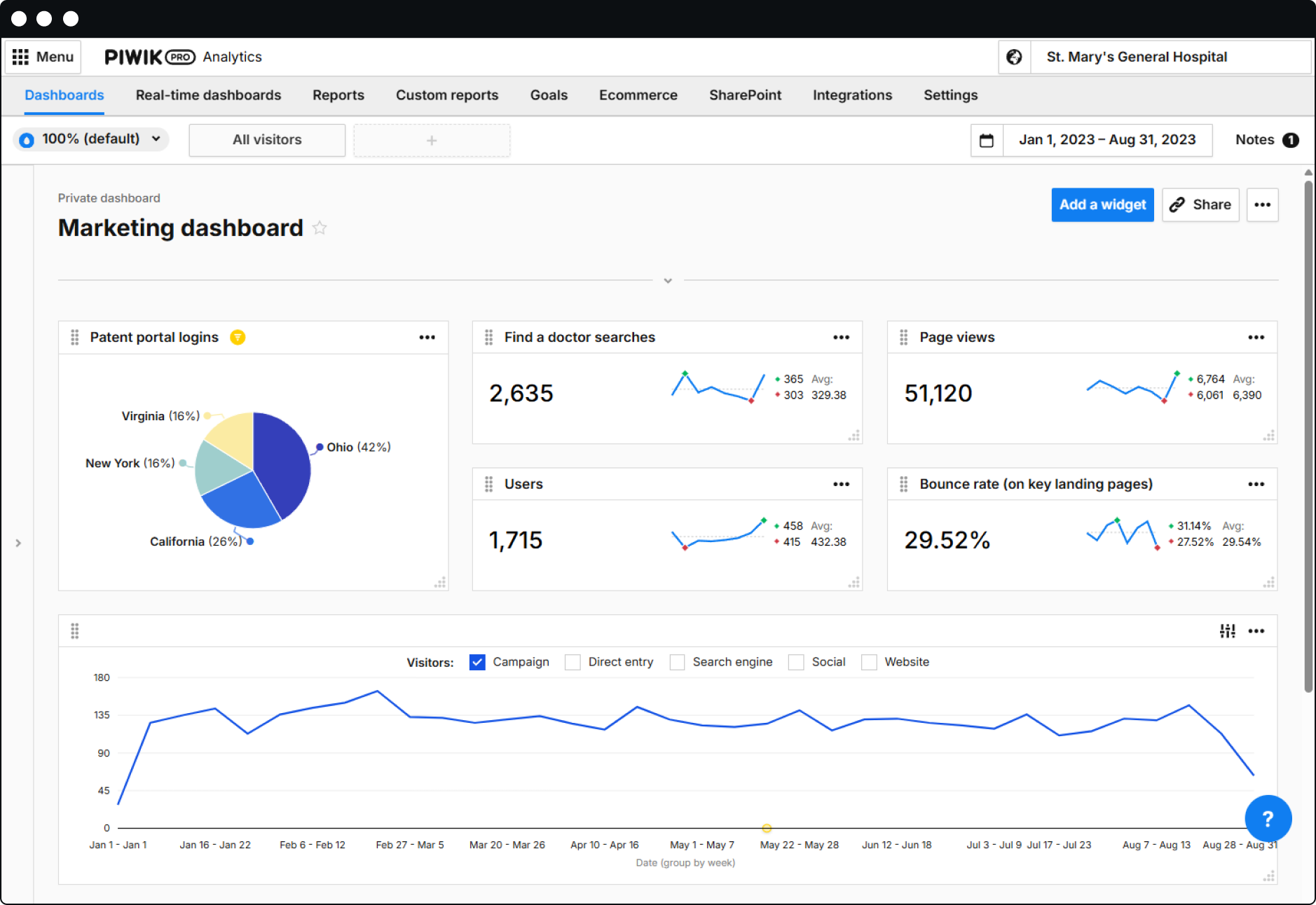






Most marketing analytics tools weren’t built for healthcare
Forcing them to work in a HIPAA environment means constant workarounds – hours spent on compliance fixes, and data gaps that make every decision harder. Piwik PRO was built to end that – so you can get up and running quickly, with complete HIPAA-safe insights and a platform your marketing team can run on their own.
Everything your legal team needs to say yes
Custom BAA, HIPAA-certified infrastructure, and built-in privacy safeguards – so your legal team can sign off with confidence.
256-bit AES encryption at rest and in transit
HIPAA-compliant Azure hosting in the US
Secure PHI collection and data anonymization
Complete data on patient acquisition
A full picture of which channels and campaigns are driving patient appointments. Get the attribution accuracy and data activation tools to turn those insights into action.
Full patient journey from search to appointment
98% attribution accuracy
Data activation capabilities
First insights in days, not months
Piwik PRO is designed to get your team up and running fast – with a familiar interface, dedicated implementation, and ongoing support to answer any questions along the way.
Marketer-friendly interface
Dedicated implementation & ongoing support
Free training resources

“I really liked how intuitive, easy, and familiar Piwik PRO felt compared to other platforms. We’re a small in-house team, so not having to onboard into a new platform that would require a very steep learning curve was very helpful for us.”
Chris Walker
Director of Digital Strategy and Marketing, Shepherd Center
Complete, HIPAA-safe marketing data – in an interface your team can use without calling IT
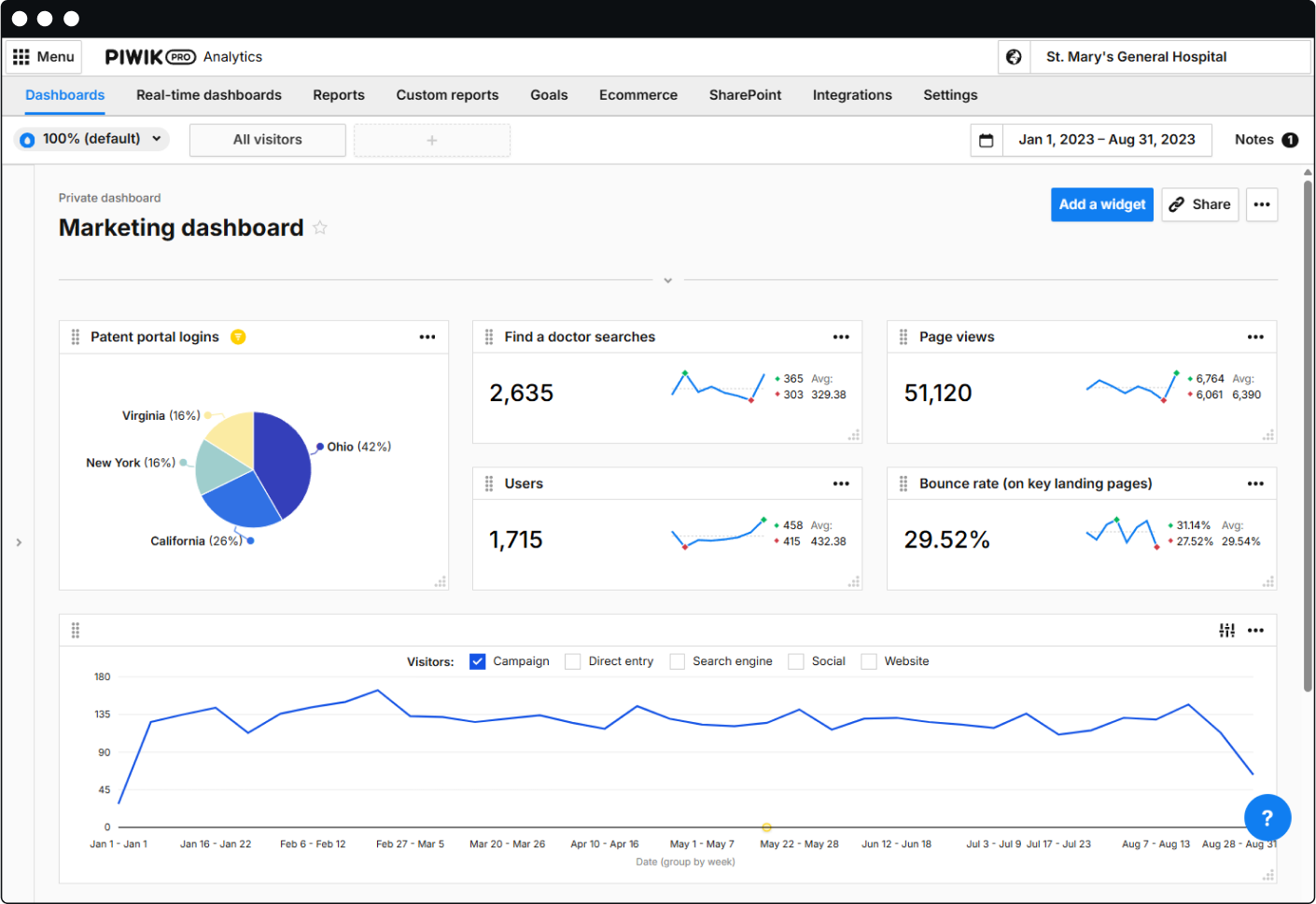
Find out what HIPAA-compliant analytics looks like for your organization
Hospitals & health systems
Track which channels and campaigns drive patient appointments across service lines – and finally have the numbers to back it up in your next leadership meeting.

Telehealth platforms
See exactly where patients drop off between symptom search and completed virtual visit – and fix it, without compromising on compliance.

Healthcare education
Track which channels drive applications, enrolments, and CME completions while meeting both FERPA and HIPAA requirements across every touchpoint.

Pharmaceutical
Measure how your disease awareness campaigns and patient support programs are really performing across HCP portals, patient education sites, and apps. Accurately, and compliantly.
What changes when healthcare marketers have data they trust
40%
Rise in online patient referrals
Shepherd Center
215%
Increase in page views
Shepherd Center
98%
Last-click attribution accuracy
Platform benchmark

Shepherd Center was using Google Analytics – which meant compliance risk and incomplete data. After switching to Piwik PRO, they got the full picture of what was driving patient acquisition and grew patient referrals by 40%.

Rochester Regional Health needed to replace Google Analytics with a platform suitable for managing patient data. With Piwik PRO, they got complete behavioral data across all their digital channels – and used it to grow their website traffic.
Analytics, tag management, and data activation – built to work together, under one BAA
Analytics
Get the complete picture of your patient acquisition funnel, SEO performance and more. Confidently attribute traffic and conversions, and learn what drives your ROI.
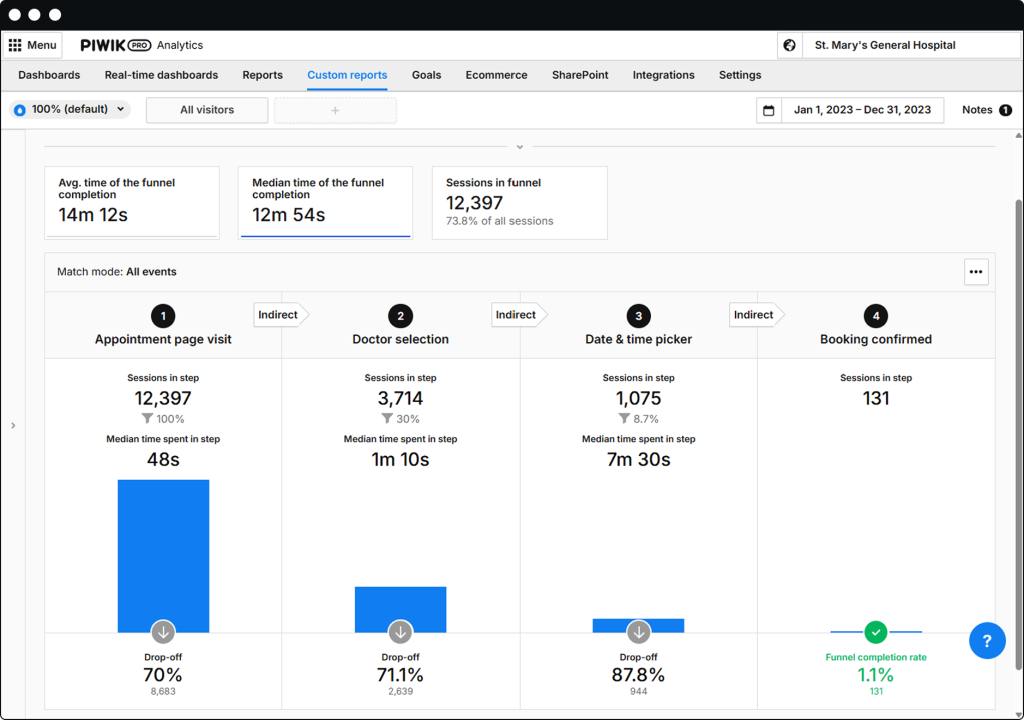
Tag Management – Collect & control
Deploy and manage your marketing tags safely – with controls that ensure that your tags and pixels fire in a HIPAA-compliant way.
Data Activation
Turn patient behavioral data into targeted email marketing campaigns, content recommendations and more. All inside an integrated HIPAA-compliant environment.

“There wasn’t any other option on the market that allowed us to capture all the data we wanted and ensure it was HIPAA-compliant.”
Tyler Pierce
Manager, Digital Engagement, Rochester Regional Health
Your path to HIPAA-compliant marketing analytics
A repeatable, guided process – so you know what to expect from day one.
Sign your BAA
A customized BAA is prepared and signed before any data collection begins.
Guided setup
Your dedicated implementation specialist sets up the platform and onboards your team.
First insights
Your team gets access to accurate, HIPAA-safe marketing analytics data.
Optimize & activate
You start making real improvements with complete, compliant insights behind every decision.
Resources on HIPAA-compliant analytics
-
We’re introducing Piwik PRO MCP Beta – get answers from your data without building a single report
We’ve just shipped MCP Beta for Piwik PRO, making it possible to query your analytics data directly through AI tools like Claude. It’s available now for early adopters. Here’s what it solves, how it works, and how to get access. Getting answers from your analytics shouldn’t feel like a research project – but it often…
-
HIPAA-compliant analytics for healthcare systems: How hospital marketing teams can measure what matters
Patients now research symptoms, compare providers, and book appointments entirely online before ever contacting a hospital. Healthcare marketers need to adapt to digital-first patient journeys, run campaigns for numerous service lines, manage hospital marketing analytics across multiple locations, and prove ROI to administrators. For nonprofit hospitals, the picture is broader still — donation tracking is…
Frequently asked questions (FAQ)
Who must follow HIPAA requirements?
HIPAA applies to covered entities, including health plans, healthcare providers that conduct business electronically, healthcare clearinghouses, and their business associates. This includes most doctors, clinics, hospitals, health insurance companies, and analytics vendors that handle protected health information (PHI).
What is PHI and ePHI under HIPAA?
Protected Health Information (PHI) is health information combined with any of the 18 HIPAA identifiers (name, address, dates, phone numbers, email, IP address, and more). Electronic PHI (ePHI) is the same information in digital format. Importantly, data collected on a healthcare website is considered PHI even if the visitor isn’t an existing patient.
Why is HIPAA compliance crucial for healthcare marketing?
By ensuring your analytics and marketing activities are HIPAA-compliant, you protect patient trust, prevent costly violations (which can result in hefty fines and lawsuits), and give you a competitive advantage over non-compliant organizations. It also ensures you can safely leverage patient data for better marketing outcomes.People now care about the privacy of their data more than ever. Health information is a special category of personal information because it contains details about users’ conditions that they may not want to disclose. Protecting the privacy of health-related data helps you maintain the trust of individuals whose information you are processingNeglecting users’ rights related to HIPAA can negatively affect your business and have a long-lasting impact on how patients view your organization. Since HIPAA is a standard that must be followed by many organizations similar to yours, the lack of compliance can make you lose business to your compliant competitors. Not to mention that any covered entity that violates HIPAA regulations can face civil action lawsuits, criminal charges, and hefty monetary penalties.
What’s included in your HIPAA-compliant analytics and data activation platform?
You get integrated analytics, tag management and data activation, all accessible through one interface with HIPAA-compliant features.
How does the business associate agreement (BAA) work?
We provide a BAA tailored to your needs, regardless of your hosting option. A BAA establishes clear responsibilities for PHI protection, ensures joint compliance, and enables you to safely collect and analyze patient data without de-identifying it.HIPAA certification proves that Piwik PRO Analytics Suite is a verified solution for customers whose policies mandate partnering exclusively with HIPAA-compliant vendors. This certification demonstrates our commitment to ensuring a HIPAA-compliant analytics suite safeguarding Protected Health Information (PHI).
How do you protect patient data?
We use 256-bit AES encryption for data at rest and in transit, HIPAA-compliant Microsoft Azure hosting in the US, comprehensive audit logs, advanced user permissions, and secure backup storage. We never share your data with third parties or use it for other purposes.Note: De-identification of PHI is not necessary with Piwik PRO – you can sign a BAA and send the desired PHI.You need to carefully select an analytics vendor that would allow you to achieve HIPAA compliance – for example, don’t forget that Google Analytics is not HIPAA compliant.You must either make an extra effort to avoid passing any trace of PHI to your analytics or switch to an analytics platform that will help you process patient data with the proper safeguards.
Can I control what happens with my data?
Yes, you maintain 100% control over your data. You can disable IP address collection, limit PHI in URLs, set granular access controls, and decide exactly what patient data you collect and how it’s used without privacy concerns.
Do I need to de-identify patient data?
No, unlike other platforms, you don’t need to de-identify PHI with Piwik PRO. A signed BAA allows you to work with complete patient data safely, providing deeper insights than competitors that require you to strip all identifiers before sending data to their platforms.
How does Piwik PRO compare to Google Analytics?
Google Analytics does not offer a BAA and is not HIPAA-compliant. Using it puts healthcare organizations at serious risk of regulatory violations and loss of patient trust. Piwik PRO provides the familiar analytics experience you’re used to, with full HIPAA compliance, a BAA tailored to your needs, and the ability to work with actual patient data rather than anonymous or fragmented information.
How does Piwik PRO compare to Freshpaint?
Freshpaint works as a data filter – it sits between your website and marketing tools like Google Analytics, stripping PHI before it’s passed on. This prevents compliance violations, but it also means your analytics are based on incomplete data from the start.
Piwik PRO takes a different approach. Instead of filtering data before it reaches third-party tools, it keeps all data – including sensitive patient information – within its own platform. Because PHI never gets shared with outside vendors, there’s no need to strip it. A signed BAA provides the legal framework to work with complete patient data safely and compliantly. The result is fuller, more accurate insights without the compliance tradeoffs that come with filtering-based solutions.




















